Infectious diseases that could lead to the next pandemic
“Throughout history, nothing has killed more human beings than the viruses, bacteria and parasites that cause disease. Not natural disasters like earthquakes or volcanoes. Not war – not even close.”
Bryan Walsh, COVID-19 the history of the pandemics
With Covid-19 in the centre of attention for nearly two years, other infectious diseases should not be left forgotten. Some of them already had a couple of outbreaks in the Covid years. Viruses like Ebola, SARS, Marburg, Monkeypox and Zika listed below are just a small portion of possible epidemic-prone viruses that could lead to the next pandemic. Being aware and prepared for the next pandemic should be our main focus for the future.
EBOLA VIRUS
What is Ebola Virus?
Ebola is a deadly infectious disease caused by viral infection. It was first discovered in 1976 near the Ebola River from where it got the name. Every now and then, an Ebola outbreak appears sporadically, mostly in African countries.
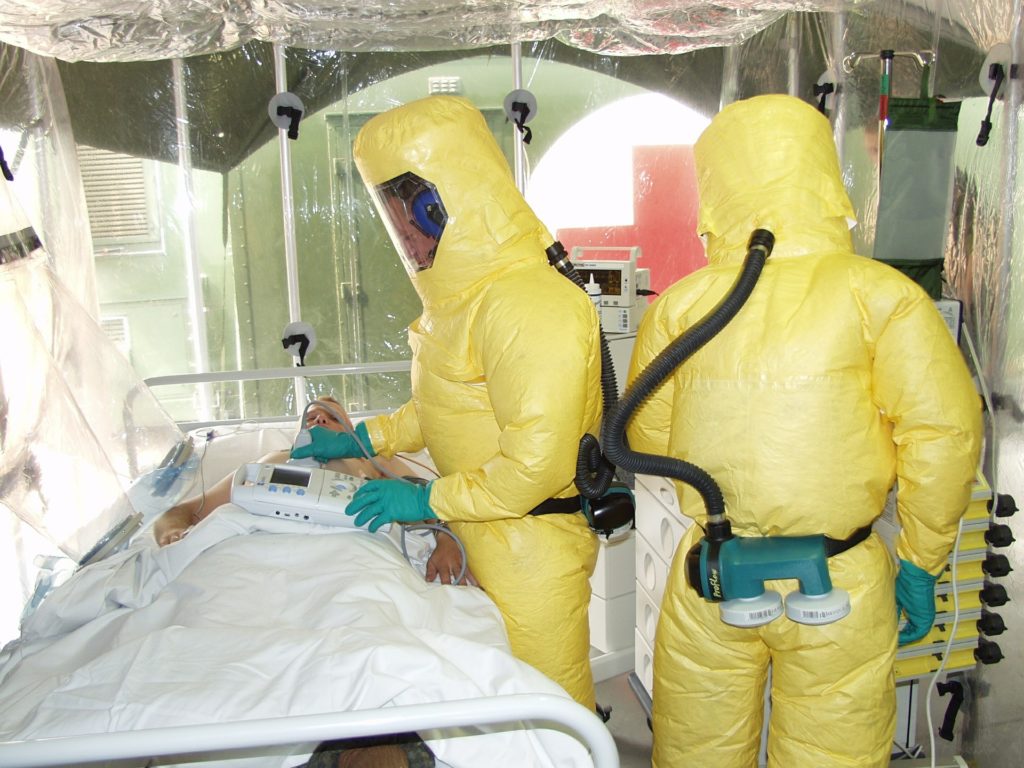
Although the risk of an outbreak in Europe or the United States is very low, healthcare professionals from Centers for Disease Control and Prevention (CDC) have taken many precautions to prevent this from happening. Immediate identification and quick response time are the best predictors for stopping the spread.
The History of Ebola outbreaks?
In February 2021, amid the coronavirus pandemic, a new outbreak of Ebola occurred. The republic of Guinea has yet again experienced an outbreak after the 2014-2016 Ebola epidemic in West Africa – a rough period that took more than 11,300 lives with mortality reaching up to 50%.
Technical committees and Ebola mitigation mechanisms deployed during the 2014–2016 Ebola epidemic gathered a lot of experience with the fight against Covid-19 pandemic and successfully put the last Ebola outbreak in 2021 under control.
What are the symptoms of Ebola virus?
In the early stages, Ebola symptoms can seem like the flu symptoms i.e.. weakness, fever, headache, sore throat, muscle pain, etc. making it hard to diagnose the virus without blood or tissue samples. As the disease gets worse, it causes bleeding inside the body and from cavities (eyes, ears, nose). Some patients can vomit or cough up blood or get bloody diarrhoea as well.
SARS (Severe Acute Respiratory Syndrome)
What is SARS virus?
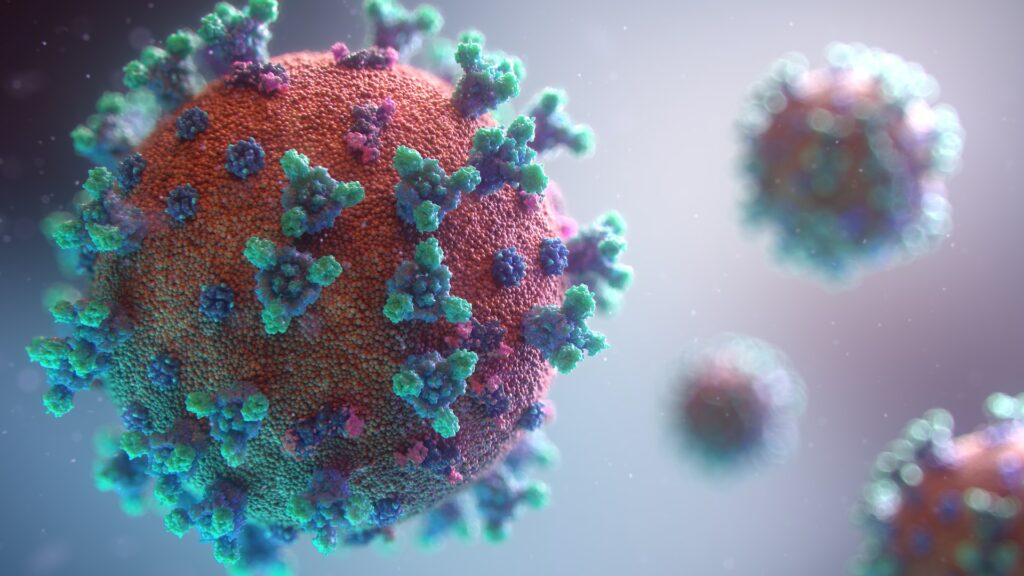
SARS is a viral respiratory infectious disease caused by SARS associated coronavirus. It originated in China in 2002. SARS outbreak emerged in February 2003 and spread quite quickly to other Asian countries. Also, there was a small number of cases in the UK and Toronto, Canada.
The history of SARS outbreaks.
There have been two SARS outbreaks which both resulted in a highly contagious form of pneumonia. As mentioned above, the first happened in 2003 and the second one in 2004. Since then, there have not been any new cases and the risk is relatively low.
Similar to SARS-Cov-2, the SARS pandemic was brought under control by isolating people with suspected disease and screening measurements of passengers travelling by air from the affected areas.
During the pandemic period, World Health Organization reported 774 deaths out of 8,098 infected, meaning the disease killed every 1 out of 10 persons who got infected. The people at risk were mostly the ones over the age of 65.
What are SARS symptoms?
SARS symptoms include high temperature, headache, muscle pain, loss of appetite, tiredness, an overall feeling of discomforT. These symptoms are quite mild compared to the ones occurring after the infection starts affecting the respiratory system (lungs and airways) like breathing difficulties, lack of oxygen in the blood and dry cough, which can be fatal in most severe cases.
There is obviously a strong connection of the “old” SARS virus with todays’ SARS-Cov-2 virus. According to Natures article the people who were infected with the virus generate a powerful antibody response after being vaccinated against COVID-19. Apparently, their immune systems can fight off multiple SARS-CoV-2 variants.
MONKEYPOX
What is Monkeypox virus?
Monkeypox is a rare illness caused by the monkeypox virus. It’s in the same viral family as smallpox. Medical scientists first discovered this infectious disease in 1958 in lab monkeys in a place called Monkeypox – hence the name.
Genomic sequencing shows there are two monkeypox clades: Congo Basin and West African with some differences in human pathogenicity and fatality. Both clades can be transmitted by contact via exhaled large droplets or via materials such as bedding.
The origin and history of Monkeypox outbreaks.
The first human infected by the virus was recorded in the Democratic Republic of Congo in 1970. The virus usually appears in forested parts of Central and West Africa but has been documented six times outside of Africa.
Not so long ago there was an outbreak of Monkeypox in the United States, a long time after the first one in 2003 when there have been reports of 47 cases. Other reported cases were in 2018 in the United Kingdom and Israel, in 2019 in Singapore, and in both the United Kingdom and the United States in 2021.
In 2022, cases of monkeypox have been reported from countries where the disease is not endemic. Most confirmed cases were reported in Europe and North America, rather than West or Central Africa where the virus is endemic. This is the first time that clusters have been reported in both non-endemic and endemic countries in disparate geographical areas.
What are the symptoms of Monkeypox?
The symptoms of monkeypox are like smallpox symptoms but a bit milder. It usually feels like catching flu and begins with a fever, chills, headache, overall exhaustion, and muscle pain. The main difference between the two poxes is that monkeypox causes swelling of lymph nodes while smallpox does not.
The infectious disease typically lasts 2-4 weeks and can be fatal and quite serious especially in younger age groups. In some cases, thousands of legions grow together and cause the loss of large skin sections all at once. According to some records, up to 10% of people who get infected die from the disease.

MARBURG VIRUS
What is Marburg virus?
Marburg virus is an “epidemic-prone” disease, meaning it can easily spread between people. It comes from Filovirus – the same family of viruses as Ebola, making it hard to distinguish between the two. Both diseases are clinically similar and rare with high fatality rates. The case fatality ratio of the Marburg virus can be up to 88% but it can be lower with proper care and treatment.
The origin and history of Marburg outbreaks.
It was first detected in 1967 in two places simultaneously, Frankfurt and Belgrade. The two outbreaks were connected to lab African green monkeys that were imported from Uganda.
However, a couple of decades later, the true origin of the virus was found – the fruit bat. It can carry the virus but not show any signs of illness. The most probable scenario was that the monkeys were infected by the infected bat, which then led to human infection.
According to WHO, human infections by the Marburg virus appear after prolonged exposure to caves or mines inhabited by Rosettus bat colonies.
On 13 February 2023, the Ministry of Health and Social Welfare of Equatorial Guinea declared an outbreak of Marburg virus disease. Since then and as of 11 April 2023, six additional laboratory-confirmed cases were reported in Equatorial Guinea.
What are the symptoms of Marburg virus?
First symptoms of Marburg virus disease are high fever, severe headache, muscle aches, abdominal pain etc. It also causes vomiting and diarrhoea that can last for a week.
Severe cases can develop hemorrhagic symptoms like bleeding from cavities including nose and gums, bleeding during vomiting, etc. Also, in most severe cases death can occur after the 8th or 9th day which is caused by blood loss and shock.

LASSA FEVER
What is Lassa fever?
Lassa fever is an acute viral hemorrhagic illness caused by the Lassa virus. It is one of the hemorrhagic fever viruses like Ebola and Marburg virus and very hard to differentiate. Unlike Ebola, Lassa is not as contagious nor as deadly.
The illness is zoonotic, or animal-borne and endemic in parts of West Africa. The host of the Lassa virus is a rodent known as a multimammate rat. Once a rodent becomes infected it can carry the disease until it dies transmitting it through urine. The transmission to humans most commonly occurs through inhalation or ingestion when the rat excretes the virus infected urine on food or materials humans use.
The origin and outbreaks of Lassa fever.
In 1969 three missionary nurses died in Lassa, a town in Nigeria, after caring for an infected patient. The particle of the virus was first described in the 1950s but was discovered and named after examining the nurses.
Every now and then there is a Lassa fever outbreak – if it can be called an outbreak – it appears simultaneously throughout the year. CDC estimates around 100,000 to 300,000 infections every year with approximately 5,000 deaths.
What are the symptoms of Lassa fever?
Signs and symptoms of Lassa fever are like Ebola or Marburg hemorrhagic fever symptoms. They typically occur 1 to 3 weeks after the person comes in contact with the virus. The majority of symptoms are quite mild and there is no need for hospitalization – 80% of infections.
Mild symptoms include general weakness, fever, and headache. However, in 20% of the infected, the virus can cause serious consequences like hemorrhaging (bleeding), respiratory difficulties, vomiting, pain in the chest, back and abdominal pain.
The most common complication found among the sick is deafness. In approximately one-third of infections, some degree of deafness appears which is not connected to the severity of the disease. Mild, as well as harsh infection, may lead to a certain degree of hearing loss or complete deafness.
ZIKA
What is Zika virus?
Zika fever is a mosquito-borne viral disease caused by the Zika virus – a virus in the flavivirus family, firstly discovered in 1947 in Uganda in monkeys. It was later in 1952 when it was identified in humans both in Uganda and the United Republic of Tanzania.
Zika infectious disease is usually transmitted by the bite of an infected Aedes mosquito living mainly in tropical and subtropical regions. Interestingly, the mosquito usually bites during the day and it is the same mosquito that transmits dengue, chikungunya and yellow fever.
The origin and history of Zika outbreaks.
The first recorded outbreak of the Zika virus was reported on the Island of Yap in 2007. It was followed by a large outbreak in French Polynesia in 2013 and other countries in the Pacific. The next one was reported in Brazil in 2015 as well as in July when it was found to be associated with Guillain-Barré syndrome.
What are the symptoms of Zika virus?
Symptoms of Zika virus are usually mild and last for several days up to a week. The majority of people who get infected don’t get sick enough for hospitalisation and fortunately, the death rate is quite low. Most mild symptoms include fever, rash, muscle and joint pain, and conjunctivitis which lasts for 2-7 days.
The biggest downside of mild, sometimes non existing symptoms is that people don’t even know that they are infected, and in some cases, later on, it can lead to complications, especially on a pregnant woman’s fetus.
How to react when viral outbreak occurs?
Despite some viruses have reported outbreaks in particular parts of the world, there is always a possibility of spreading like SARS-Cov-2. More epidemic-prone viruses are more likely to spread the disease in large scale than others, but the fear is always present.
The best way of mitigating the outbreaks is to be prepared for the next possible pandemics with various precaution measures which include having the right equipment at hand. The EpiShuttle has been used all around the world and has been recognised as a preferred solution for infection isolation and transport.
EpiShuttle can help with the preparedness and stop the spread of viral diseases by “Saving one – Protecting everyone”.